The immune system is designed to detect and eliminate abnormal cells, including cancer. Specialized immune cells such as T cells and natural killer (NK) cells constantly patrol the body, identifying threats and destroying damaged or mutated cells before they can form tumors.
This process, known as immune surveillance, is one of the body’s most powerful defenses against cancer. In many cases, the immune system successfully eliminates cancer cells before they are ever detected.
However, cancer does not passively exist. Tumors actively evolve mechanisms to survive, grow, and evade destruction. One of the most important and dangerous strategies tumors use is immune exhaustion—a state in which T cells lose their ability to function effectively.
Immune exhaustion explains why the immune system can be present around tumors yet fail to eliminate them. It is also one of the key reasons why modern immunotherapy treatments, such as checkpoint inhibitors, have become revolutionary in cancer care.
The Role of T Cells in Fighting Cancer
T cells are a central component of the adaptive immune system and play a critical role in identifying and destroying cancer cells.
When cells become abnormal due to mutations, they display unusual proteins called antigens on their surface. T cells recognize these antigens as dangerous and initiate an immune response.
Types of T Cells Involved
Cytotoxic T cells (CD8+)
These directly attack and kill cancer cells by releasing toxic enzymes.
Helper T cells (CD4+)
These coordinate immune responses and activate other immune cells.
Memory T cells
These allow the immune system to respond faster if the same threat appears again.
When functioning properly, T cells can prevent tumor formation entirely. However, cancer can disrupt this process.
For a deeper understanding, see:
https://helping4cancer.com/cancer-immune-system/
What Is Immune Exhaustion?
Immune exhaustion is a state where T cells become progressively less effective after prolonged exposure to cancer cells.
Unlike short-term infections, cancer can persist for months or years. This continuous stimulation overwhelms T cells and gradually reduces their functionality.
Key Features of Exhausted T Cells
• Reduced ability to kill tumor cells
• Decreased cytokine production
• Limited proliferation
• Increased expression of inhibitory receptors
These changes result in weakened immune responses, allowing cancer cells to survive and grow.
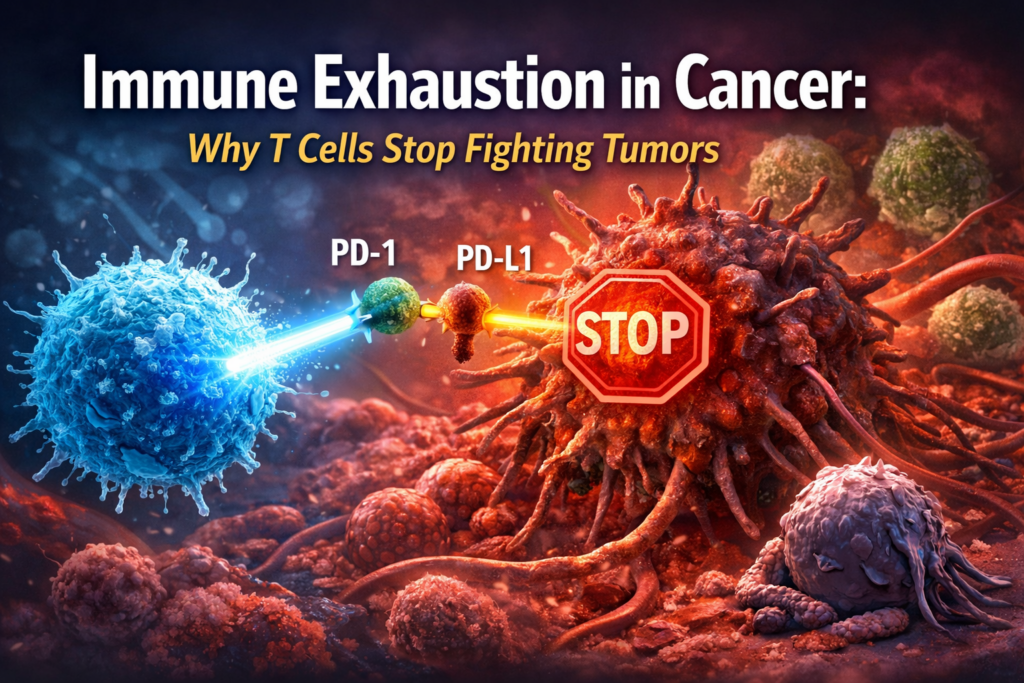
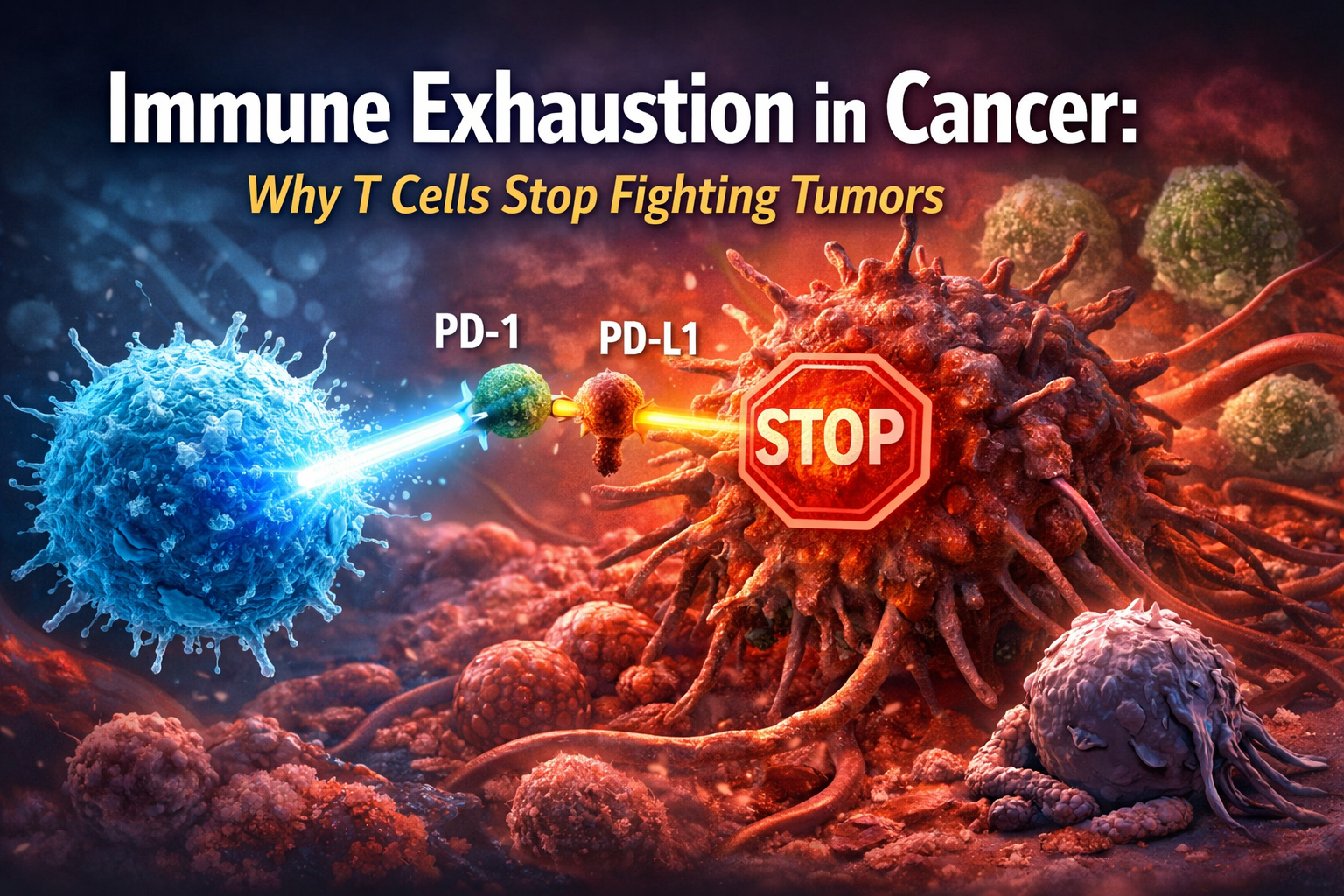
PD-1: The Immune System Brake
One of the most important drivers of immune exhaustion is the PD-1 (programmed cell death protein-1) pathway.
PD-1 is a receptor found on T cells that acts as a regulatory checkpoint. Its role is to prevent the immune system from becoming overactive and damaging healthy tissue.
How PD-1 Works
When PD-1 binds to its partner protein PD-L1, a signal is sent that reduces T cell activity. This is a normal and necessary mechanism for immune balance.
However, cancer cells exploit this system.
How Tumors Use PD-1 Against the Immune System
Many tumors express high levels of PD-L1 on their surface. When PD-L1 binds to PD-1 on T cells, it effectively sends a message to stop attacking.
This allows cancer cells to:
• Avoid immune destruction
• Create a protective environment
• Promote long-term survival
Over time, repeated activation of PD-1 signaling leads to T cell exhaustion.
Immune Suppression in the Tumor Microenvironment
Immune exhaustion does not occur alone. It is part of a broader process involving the tumor microenvironment (TME).
The tumor microenvironment includes all surrounding cells, signaling molecules, and structures that interact with the tumor.
Tumors actively modify this environment to suppress immune responses.
Key Mechanisms of Immune Suppression
Chronic Antigen Exposure
Constant stimulation of T cells leads to functional decline over time.
Suppressive Immune Cells
Tumors recruit cells that weaken immune responses, including:
• Regulatory T cells (Tregs)
• Myeloid-derived suppressor cells (MDSCs)
Inhibitory Cytokines
Tumors release signaling molecules such as:
• TGF-β
• IL-10
These suppress immune activity and reduce T cell effectiveness.
Metabolic Competition
Cancer cells consume large amounts of glucose and nutrients, depriving immune cells of energy.
Learn more about this here:
https://helping4cancer.com/tumor-microenvironment-explained/
Immune Checkpoints and T Cell Exhaustion
PD-1 is only one of several immune checkpoints involved in exhaustion.
Other Important Checkpoints
CTLA-4
Regulates early stages of T cell activation.
LAG-3
Contributes to long-term immune suppression.
TIM-3
Associated with severely exhausted T cells.
Exhausted T cells often express multiple checkpoints simultaneously, making them even less effective.
Checkpoint Inhibitors: Turning the Immune System Back On
One of the most important breakthroughs in cancer treatment is the development of checkpoint inhibitors.
These drugs block inhibitory signals like PD-1 or PD-L1, allowing T cells to regain their function.
How Checkpoint Inhibitors Work
• Block PD-1 or PD-L1 interaction
• Remove the “off” signal
• Reactivate T cell killing ability
Common Checkpoint Inhibitors
• Pembrolizumab
• Nivolumab
• Atezolizumab
• Ipilimumab
These therapies have significantly improved outcomes in several cancers, including:
• Melanoma
• Lung cancer
• Kidney cancer
• Bladder cancer
For more on immune evasion:
https://helping4cancer.com/tumor-immune-escape-mechanisms/
Why Immunotherapy Does Not Work for Everyone
Despite their success, checkpoint inhibitors are not effective in all patients.
Key Factors Influencing Response
Tumor Mutation Burden
More mutations create more recognizable targets for T cells.
PD-L1 Expression
Higher PD-L1 levels often increase response to therapy.
Immune Cell Presence
“Hot” tumors with immune cells respond better than “cold” tumors.
Tumor Metabolism
Cancer metabolism can weaken immune function.
Explore metabolism further:
https://helping4cancer.com/cancer-metabolism-explained/
The Link Between Metabolism and Immune Exhaustion
Cancer cells require large amounts of energy and nutrients.
They consume:
• Glucose
• Glutamine
• Iron
This deprives immune cells of the resources they need to function properly.
How This Affects T Cells
• Reduced energy production
• Impaired signaling
• Decreased survival
This metabolic competition contributes directly to immune exhaustion.
Related topics:
https://helping4cancer.com/cancer-cells-love-sugar/
https://helping4cancer.com/cancer-cells-need-iron/
Can Exhausted T Cells Recover?
One of the most important discoveries in cancer immunology is that immune exhaustion may be partially reversible.
Checkpoint inhibitors can restore T cell activity in some cases.
Factors That Influence Recovery
• Severity of exhaustion
• Tumor microenvironment conditions
• Immune diversity
• Metabolic support
However, not all exhausted T cells can be fully restored, which is why combination therapies are being explored.
Future Strategies to Overcome Immune Exhaustion
Researchers are developing new approaches to enhance immune responses.
Emerging Approaches
Combination Immunotherapy
Targeting multiple checkpoints at once.
Metabolic Therapy
Improving immune cell energy availability.
Cancer Vaccines
Training the immune system to recognize tumors.
Cellular Therapies (CAR-T)
Engineering immune cells to better target cancer.
These strategies aim to overcome immune suppression and improve long-term outcomes.
Why Immune Exhaustion Matters
Immune exhaustion is one of the most important concepts in modern cancer biology.
It explains why tumors can survive despite an active immune system and highlights how cancer actively suppresses immune function.
By understanding immune exhaustion, researchers have developed therapies that restore immune activity and improve survival in many patients.
Checkpoint inhibitors represent a major shift in cancer treatment—focusing not just on killing cancer directly, but on empowering the immune system to do the job.
Key Takeaways
• Immune exhaustion weakens T cells and limits their ability to kill cancer
• PD-1 and PD-L1 interactions suppress immune responses
• Tumors actively create an immunosuppressive environment
• Checkpoint inhibitors can restore immune function
• Future therapies aim to further enhance immune responses
External References
National Cancer Institute
https://www.cancer.gov
Nature Reviews Cancer
https://www.nature.com
Cancer Research Institute
https://www.cancerresearch.org
ScienceDirect
https://www.sciencedirect.com
Table of Contents