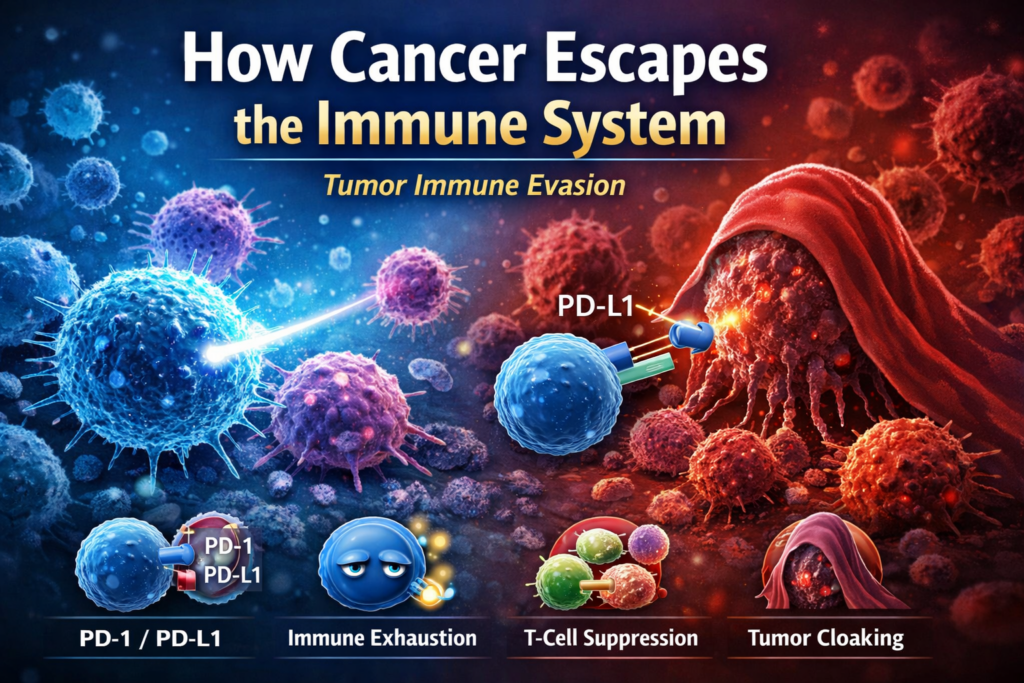
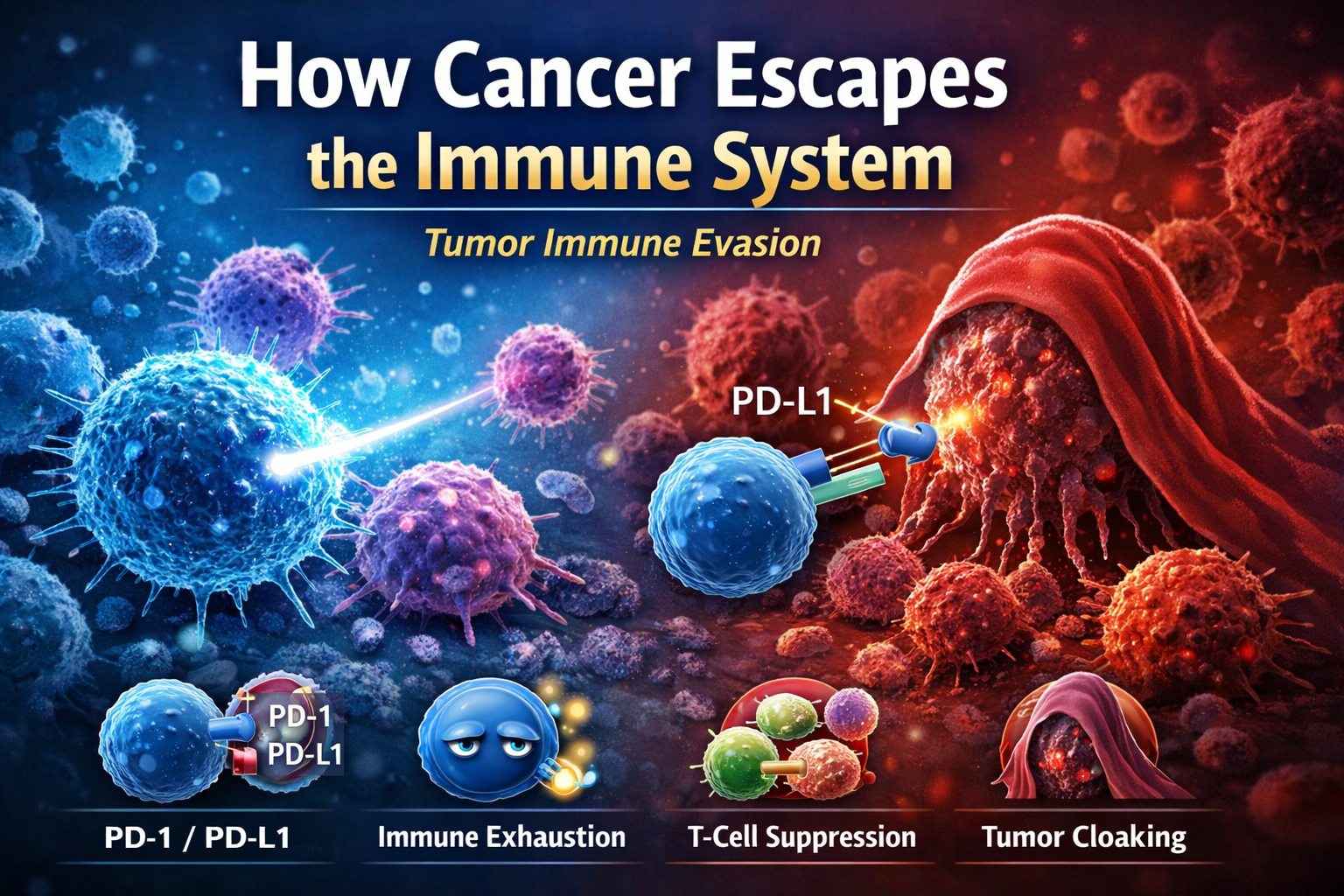
Tumor Immune Escape Mechanisms Explained
The human immune system constantly searches for abnormal cells. Every day, natural killer (NK) cells and cytotoxic T-cells identify and destroy potentially dangerous cells before they become tumors.
This process is known as immune surveillance.
However, cancer is not simply uncontrolled cell growth. It is also an evolutionary battle between tumor cells and the immune system. As tumors develop, they acquire biological strategies that allow them to hide, suppress, or disable immune defenses.
These strategies are called tumor immune escape mechanisms.
Understanding how cancer evades immune detection has become one of the most important areas of modern oncology. Many breakthrough treatments, including immune checkpoint inhibitors, were developed specifically to overcome these escape strategies.
This guide explains the most important ways cancer avoids immune destruction.
The Battle Between Cancer and the Immune System
When abnormal cells first appear, the immune system often eliminates them before tumors can form.
Key immune defenders include:
• Natural killer (NK) cells
• Cytotoxic T cells (CD8+ T cells)
• Macrophages
• Dendritic cells
These immune cells identify threats using antigens, small molecular signals displayed on cell surfaces.
If a cell appears abnormal, immune cells can:
• trigger apoptosis (cell death)
• release cytotoxic molecules
• activate additional immune responses
However, cancer cells mutate rapidly. Over time, they may develop ways to avoid detection or disable immune attacks.
This transition from immune control to immune escape is known as immunoediting.
Learn more:
Immune Surveillance and Cancer
https://helping4cancer.com/immune-surveillance-cancer/
PD-1 and PD-L1: The Immune Checkpoint Switch
One of the most important tumor escape mechanisms involves immune checkpoint signaling.
Immune checkpoints are regulatory pathways that prevent the immune system from attacking normal healthy tissue.
One of the most important checkpoint systems involves:
PD-1 (Programmed Death-1)
PD-L1 (Programmed Death Ligand-1)
How PD-1 / PD-L1 Works
PD-1 is a receptor found on T cells, while PD-L1 is a ligand that can be expressed on other cells.
When PD-1 binds to PD-L1, the immune system receives a signal to stop attacking.
Normally this protects healthy tissues from autoimmune damage.
Cancer cells exploit this system.
Many tumors produce large amounts of PD-L1, effectively sending a “do not attack” signal to T cells.
As a result:
• T cells become inactive
• immune attacks stop
• the tumor continues growing
This mechanism is one of the most common immune escape strategies used by tumors.
Immunotherapy Targeting PD-1
Modern immunotherapy drugs block this checkpoint interaction.
Examples include:
• pembrolizumab
• nivolumab
• atezolizumab
These drugs allow T cells to recognize and attack tumors again.
Research:
National Cancer Institute
https://www.cancer.gov/about-cancer/treatment/types/immunotherapy/checkpoint-inhibitors
Immune Exhaustion
Another major tumor escape mechanism is immune exhaustion.
When immune cells fight cancer for long periods, they can become functionally exhausted.
Exhausted T cells show several changes:
• reduced killing ability
• lower cytokine production
• decreased proliferation
• increased inhibitory receptors
These exhausted immune cells remain present but lose their ability to destroy tumors effectively.
Tumors actively promote this exhaustion state.
Why Immune Exhaustion Happens
Several factors contribute to immune exhaustion:
Chronic Antigen Exposure
Constant exposure to tumor antigens causes T cells to become overstimulated.
Over time, their response weakens.
Inhibitory Receptors
Exhausted T cells express high levels of receptors such as:
• PD-1
• CTLA-4
• TIM-3
• LAG-3
These receptors suppress immune activity.
Tumor Microenvironment
The tumor microenvironment contains many immunosuppressive signals that weaken immune responses.
Learn more:
Tumor Microenvironment Explained
https://www.cancer.gov/research/areas/tumor-microenvironment
T-Cell Suppression by Tumors
Cancer cells can actively suppress immune cells.
This suppression often occurs through immune-modulating molecules released by tumors.
Key immunosuppressive factors include:
• TGF-β (transforming growth factor beta)
• IL-10 (interleukin-10)
• VEGF (vascular endothelial growth factor)
These molecules alter immune behavior in several ways.
How Tumors Suppress T Cells
Blocking T-Cell Activation
Some tumor signals prevent T cells from becoming fully activated.
Without proper activation, T cells cannot destroy cancer cells.
Recruiting Regulatory T Cells
Tumors often recruit regulatory T cells (Tregs).
These specialized immune cells suppress immune responses.
While Tregs normally prevent autoimmune disease, tumors hijack them to protect themselves.
Disrupting Dendritic Cells
Dendritic cells help activate T cells.
Cancer can disrupt dendritic cell function, preventing proper immune signaling.
As a result, the immune system becomes less effective at recognizing tumors.
Tumor Cloaking: Hiding From the Immune System
Another escape mechanism is tumor cloaking.
Cancer cells may hide from immune detection by altering how their surface appears to immune cells.
Reduced Antigen Presentation
Normal cells display protein fragments on molecules called MHC (major histocompatibility complex).
These molecules allow T cells to detect abnormal cells.
Many tumors reduce or eliminate MHC expression.
Without MHC signals, T cells cannot recognize the cancer cell.
Molecular Camouflage
Some tumors mimic normal cells by expressing molecules that suppress immune detection.
These include:
• CD47 (“don’t eat me” signal)
• PD-L1
• surface glycoproteins
CD47 is particularly important because it prevents macrophages from engulfing tumor cells.
Research:
Stanford Medicine – CD47 cancer research
https://med.stanford.edu/cancer/research/cd47.html
The Tumor Microenvironment
Cancer does not exist alone.
Tumors create a surrounding ecosystem called the tumor microenvironment (TME).
The TME contains:
• immune cells
• fibroblasts
• blood vessels
• inflammatory molecules
• signaling proteins
Many of these components actually help tumors evade the immune system.
Immunosuppressive Cells in the Tumor Microenvironment
Several cell types weaken immune responses:
Regulatory T Cells (Tregs)
Suppress cytotoxic immune activity.
Myeloid-Derived Suppressor Cells (MDSCs)
Block T-cell activation and promote tumor growth.
Tumor-Associated Macrophages (TAMs)
These macrophages can switch to a tumor-supporting state that promotes:
• angiogenesis
• tissue remodeling
• immune suppression
Together these cells create an environment where cancer can grow while immune defenses remain weakened.
Why Tumor Immune Escape Matters
Tumor immune escape is one of the central hallmarks of cancer.
Without immune evasion, most cancers would be destroyed early in their development.
Understanding these escape strategies helps researchers develop new treatments.
Many modern therapies aim to restore immune function.
Examples include:
• checkpoint inhibitors
• cancer vaccines
• CAR-T cell therapy
• NK-cell therapies
These treatments attempt to reactivate the immune system so it can eliminate cancer cells again.
The Future of Cancer Immunotherapy
Cancer immunotherapy has transformed oncology over the past decade.
Instead of attacking tumors directly, these treatments empower the immune system to do the work.
Scientists are now studying new strategies including:
• dual checkpoint inhibitors
• NK-cell activation therapies
• tumor vaccines
• personalized immune treatments
As researchers better understand tumor immune escape mechanisms, treatments will continue improving.
Many experts believe the future of oncology will involve combining immune therapy with metabolic and targeted treatments.
Key Takeaways
Tumor immune escape is one of the most important concepts in modern cancer biology.
Cancer survives by developing ways to hide from or disable immune defenses.
Major immune escape strategies include:
• PD-1 / PD-L1 checkpoint signaling
• immune exhaustion
• T-cell suppression
• tumor cloaking and antigen loss
• immunosuppressive tumor microenvironments
These mechanisms allow cancer cells to survive even when immune defenses are present.
Fortunately, modern immunotherapy treatments are designed specifically to overcome these escape strategies.
Understanding how tumors evade the immune system is a critical step toward developing more effective cancer treatments.
External References
National Cancer Institute – Immunotherapy
https://www.cancer.gov/about-cancer/treatment/types/immunotherapy
Nature Reviews Cancer – Tumor immune evasion
https://www.nature.com/articles/nrc3239
Stanford Medicine – CD47 and cancer immune escape
https://med.stanford.edu/cancer/research/cd47.html
Cancer Research Institute – Immune checkpoints
https://www.cancerresearch.org/immunotherapy
Table of Contents